Resubmit Claims Rejected by Clearinghouse
When claims are rejected by the clearinghouse, PracticeQ makes it easy to correct and resubmit them.
IMPORTANT NOTES ABOUT CLEARINGHOUSE REJECTIONS:
- PracticeQ receives information from Office Ally and TriZetto when a claim is rejected or denied, but that information may be limited.
- When claims are rejected or denied and the reasoning is unclear, PracticeQ Support recommends reaching out to the Clearinghouse to obtain more information. This ensures that you make the proper corrections before resubmission.
- Click Lists → Claims to review your claim statuses.
- Any claim rejected by the clearinghouse (Office Ally or TriZetto) will display a red rejected label in the Status column.
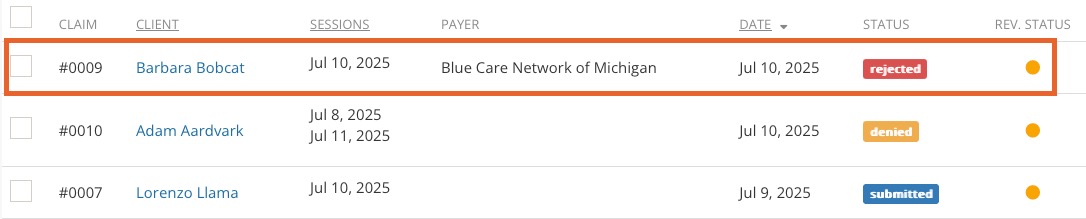
- Open the rejected claim.
- Open the Actions menu at the bottom of the claim and select Edit Claim.
- Edit the fields that require correction.
- Resubmit the claim.
Note: No reference number is required to resubmit claims rejected by the clearinghouse.
.png)
