Manually Add Insurance Payments
PracticeQ allows you to create claims and track insurance payments. When you submit claims using our Office Ally or TriZetto integrations, insurance payments are recorded and allocated automatically as payers make ERA reports available. If you work with payers who do not provide ERA reports, or if you do not use one of our clearinghouse integrations, you can record these payments manually.
To add an insurance payment, you will likely need the EOB (Explanation of Benefits) received from the insurance payer, showing you the amounts for each claim and its items. To record the payment, follow the steps below:
- Click Lists → Claims.
- Click the Payments tab.
- Click Add Payment.
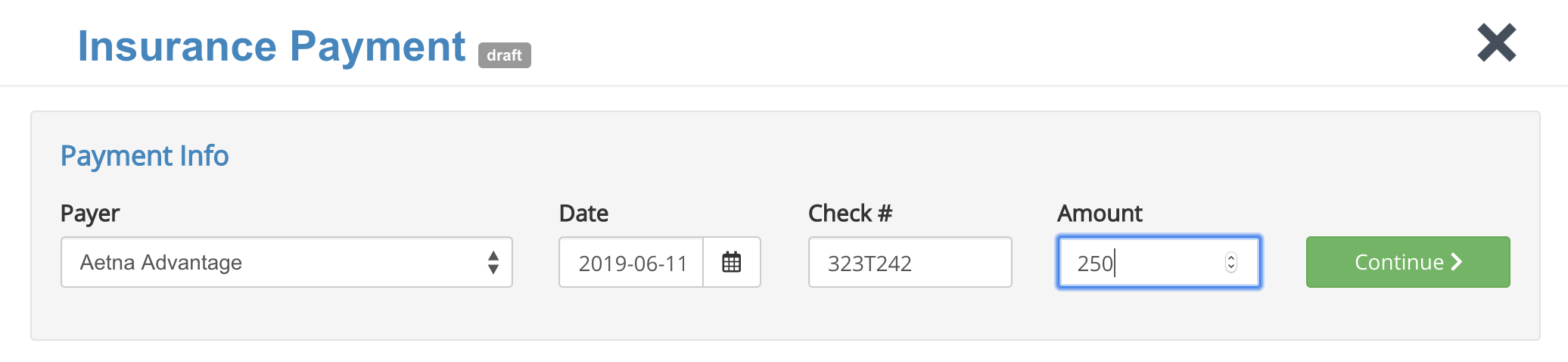
- Complete the payment information (Payer, Date, Check Number and Amount).
- Click Continue.
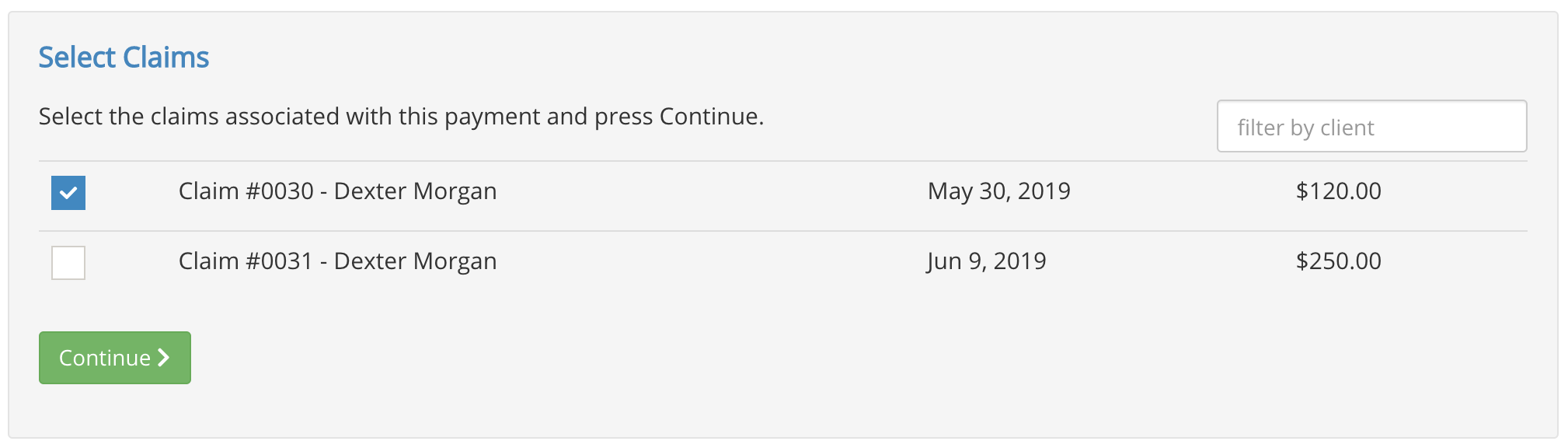
- PracticeQ will show you all claims for that payer that have been submitted but not paid. Check the claim(s) included in this EOB.
- Click Continue.
- Next, PracticeQ will show you a table that lets you allocate the EOB amounts to each claim line item, including Copay, Coinsurance and Deductibles.
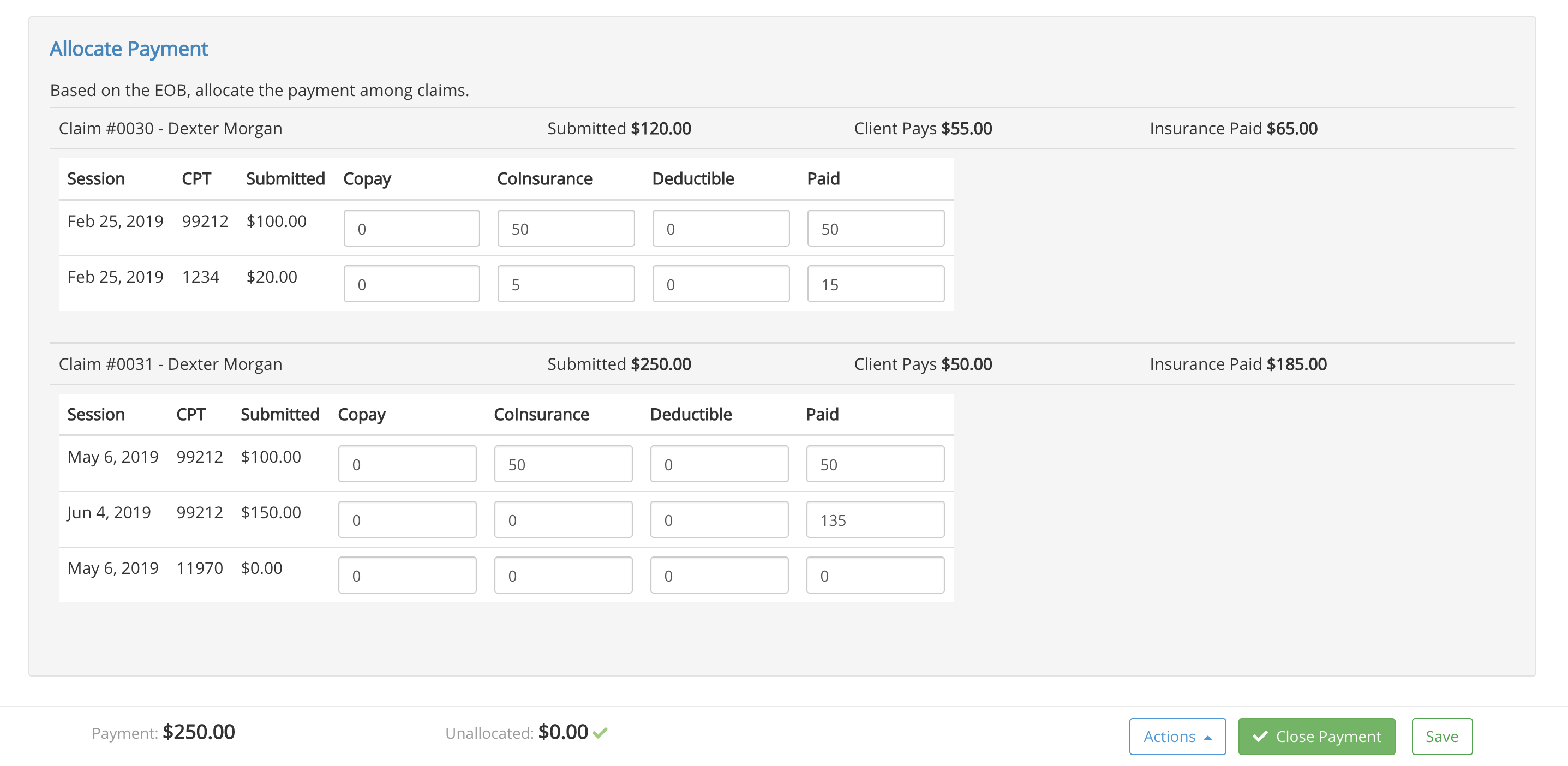
9. Note that the amounts in the Paid column should add up to the total payment amount on the bottom left. The system will display the un-allocated amount at the bottom and once that amount reaches zero, you will be able to click Close Payment.
When the payment is closed, PracticeQ will change the status on the claims and update the client responsibility on the appointments associated with these claims.
.png)